Lung Cancer Story Corner
During this challenging time, we want to inspire HOPE.

Robin Scharf | Niskayuna, NY
Cancer and Coronavirus both have similar silver linings. Life is unpredictable, and I will do my best to live well each day I am given with gratitude and appreciation. – Robin

1
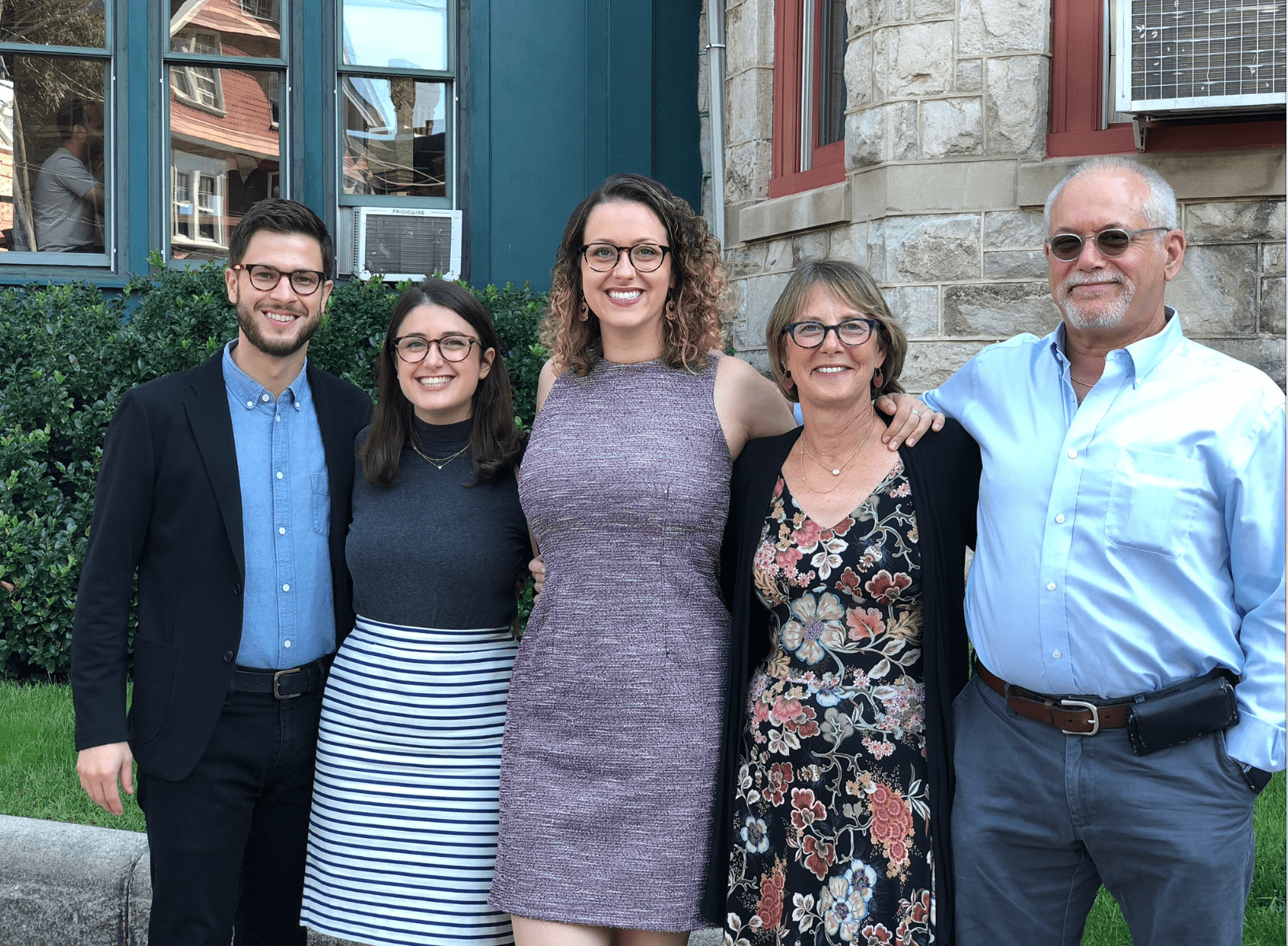 Telling my story is somewhat therapeutic. It is a lonely journey when you are faced with a serious illness, even with having a wonderfully supportive family. As a professional therapist, I listen to lots of people’s stories. My work has been a great distraction from my challenges. When a client shares how upset they are about a family member becoming ill, I tell them to slow down and not jump to conclusions. Most of all, I tell them to live in the moment because, ultimately, that is all we have. I practice mindfulness regularly since losing my friend of 49 years to ovarian cancer. When we were facing her death, we decided we had to learn to live as well as we could at the moment, as the future was too uncertain and not here yet. Our anxiety was ruining the time we had left, and we worked very hard to stay in the present.
Telling my story is somewhat therapeutic. It is a lonely journey when you are faced with a serious illness, even with having a wonderfully supportive family. As a professional therapist, I listen to lots of people’s stories. My work has been a great distraction from my challenges. When a client shares how upset they are about a family member becoming ill, I tell them to slow down and not jump to conclusions. Most of all, I tell them to live in the moment because, ultimately, that is all we have. I practice mindfulness regularly since losing my friend of 49 years to ovarian cancer. When we were facing her death, we decided we had to learn to live as well as we could at the moment, as the future was too uncertain and not here yet. Our anxiety was ruining the time we had left, and we worked very hard to stay in the present.
2
When I was in my thirties, I developed a cough that wouldn’t go away. As a precaution, the doctor took an x-ray and discovered that I had a large “something” in my chest. It turned out to be benign, but it was ominous looking. It turned out to be a bronchogenic cyst, which I was probably born with, although it had never been noticed before (even when I had back surgery). Nonetheless, they were concerned that it could open up and cause an infection. They felt it needed to be drained, so I had surgery to do so.
About six months later, during a follow-up, it reoccurred. At that point, I was told that I would have to live with it, but it should be checked regularly. For ten years, I had CAT scans yearly to see that the cyst was still there and had not changed. Finally, I asked if we could stop doing CAT scans as I was concerned about the radiation, and the cyst was stable and not causing any problems for me.
3
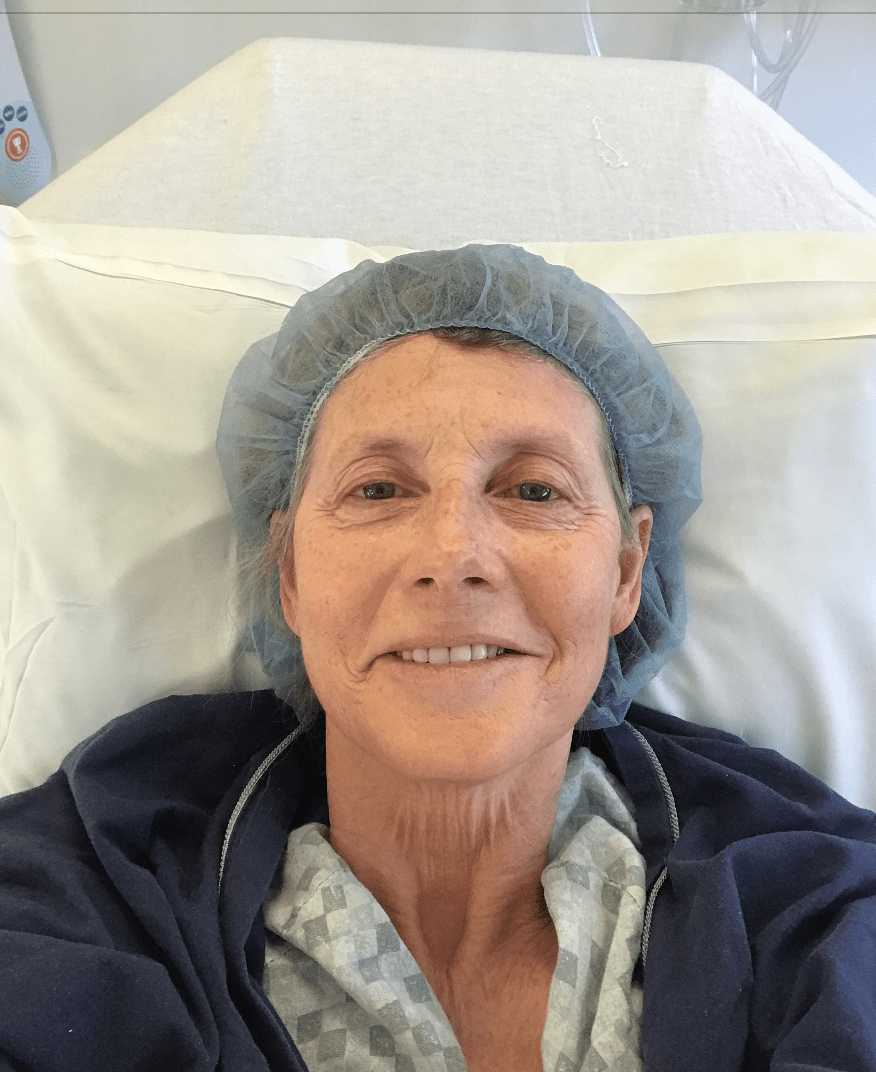 Fast forward to twenty years later. I was having some trouble with feeling like I couldn’t breathe during a particular stage of the sleep cycle. They felt it was probably related to acid reflux, but as a precaution, my doctor felt we should do a CAT scan to be sure the cyst had not changed. It was time for me to have gratitude for having that bronchogenic cyst as it made them examine my lungs. I had no symptoms of any sort related to lung cancer. I did not have a cough. I did not have any trouble with breathing. The results of the CAT scan showed that the cyst was GONE, but instead, they saw something on my lung. In my naiveté, I thought the cyst had opened, and the remnants were on my lung. They saw what they described as ‘ground-glass opacities’. I had them biopsied and was so relieved when it turned out to be benign. We watched them for a year and then they changed. I was told that the only way to be sure about what it was, was to do surgery and remove it if it was cancer. Surgery number one took place in June of 2017. The spot turned out to be adenocarcinoma, and out came my upper right lobe. It was done laparoscopically, and although I recovered well, it was a most unpleasant experience. I have had spinal surgery and was in a body cast for three months, and I can say that having a chest tube for three days was almost as bad.
Fast forward to twenty years later. I was having some trouble with feeling like I couldn’t breathe during a particular stage of the sleep cycle. They felt it was probably related to acid reflux, but as a precaution, my doctor felt we should do a CAT scan to be sure the cyst had not changed. It was time for me to have gratitude for having that bronchogenic cyst as it made them examine my lungs. I had no symptoms of any sort related to lung cancer. I did not have a cough. I did not have any trouble with breathing. The results of the CAT scan showed that the cyst was GONE, but instead, they saw something on my lung. In my naiveté, I thought the cyst had opened, and the remnants were on my lung. They saw what they described as ‘ground-glass opacities’. I had them biopsied and was so relieved when it turned out to be benign. We watched them for a year and then they changed. I was told that the only way to be sure about what it was, was to do surgery and remove it if it was cancer. Surgery number one took place in June of 2017. The spot turned out to be adenocarcinoma, and out came my upper right lobe. It was done laparoscopically, and although I recovered well, it was a most unpleasant experience. I have had spinal surgery and was in a body cast for three months, and I can say that having a chest tube for three days was almost as bad.
I recovered well and regained my lung capacity, but I promised myself I would never undergo surgery again.
4
Year one follow-up looked good. Year two follow-up looked good, and then six months later, it did not look so good. A new growth appeared in my lower right lobe. I weighed having surgery vs. radiation, but I was once again told that surgery was the gold standard, and I decided to do it again. It’s amazing how we forget what we don’t want to remember. This time, I decided to go to Sloan Kettering rather than my local upstate NY hospital, hoping that they could handle operating on an already altered lung. I was hoping to keep a portion of my lower lobe as I was told I would have to lose the whole lung if the lower lobe came out. A middle right lobe has a poor chance of doing well on its own.
Unfortunately, the unexpected happened. As the doctor was removing the growth laparoscopically, one of the instruments got stuck on a branch of my pulmonary artery, and I started to bleed out. A small laparoscopic incision became a relatively large incision to save my life. The recovery would be harder, but even harder was waking up to a pandemic while being in a hospital in the middle of New York City. The surgery was on March 11, 2020. My family was much more aware of all that was changing. All I knew was that I suddenly couldn’t have more than one visitor in one day, and they were discharging me before I felt ready.
5
I have an amazingly supportive family consisting of my husband and two adult daughters. They all came to be with me for the surgery. All my family could think about was how to get me out of the city safely and quickly. I was discharged less than 30 hours after the surgery and was in a car heading back to upstate New York one day later. I had a mask on, Purell in every pocket and fear that we couldn’t stop to go to the bathroom or get gas without exposing me to danger. Arriving back home was a major relief. It is now ten weeks later; the world has changed. I stayed in the house at all times and stayed away from all people. Waking up in the middle of a pandemic was shocking. I think I had a sense of it before we drove to NYC as I saw some evidence on my computer of seeking hand sanitizer before we drove to the city. Going back to the hotel following the surgery was somewhat surreal. No longer was it okay to touch anything or hug my family. We suddenly realized we had to get home safely, but we also had to get a supply of masks, toilet paper, and sanitizers before returning home. Having just had surgery on my lung was secondary to what we now had to face. I guess one could say it was a good distraction; however, I would have gladly done without it.
It is now ten weeks later; the world has changed. I stayed in the house at all times and stayed away from all people. Waking up in the middle of a pandemic was shocking. I think I had a sense of it before we drove to NYC as I saw some evidence on my computer of seeking hand sanitizer before we drove to the city. Going back to the hotel following the surgery was somewhat surreal. No longer was it okay to touch anything or hug my family. We suddenly realized we had to get home safely, but we also had to get a supply of masks, toilet paper, and sanitizers before returning home. Having just had surgery on my lung was secondary to what we now had to face. I guess one could say it was a good distraction; however, I would have gladly done without it.
6
When I recovered the first time, I had visitors and the support of my family and friends. I still had that support, but all of the family and friends were dealing with a changing world as well. I have been amazed at how supportive the simple actions of others can be.
When I had my last birthday, I raised money on Facebook for the Lung Cancer Research Foundation. I set my goals at $250.00. Two weeks later, and over $3000.00 raised, I felt the support of my community.
I know I am at risk. My doctor has told me that I would be at risk of not “making it” if I got COVID, and so I take one day at a time. That is nothing new to me. I already feel like I am on borrowed time, but I am determined to do all I can to stay safe and get well. Of course, getting well means walking and exercising.
6b
 As time passes and I get stronger and stronger, I am doing all I can to stay safe and regain my strength so that I would have a fighting chance of “making it.” I have a great appreciation for receiving “MY CHOICES: A Planner for Healing” as it helped me to remember who I am other than being defined by my cancer. It helped me to remember which things I had control over in light of so many things happening to me personally as well as the world around me. It may be a changing world, but I still want to be around to attend my daughter’s wedding and to see my other daughter graduate medical school. I feel blessed that my cancer was discovered early enough to remove it. Cancer and Coronavirus both have similar silver linings. Life is unpredictable, and I will do my best to live well each day I am given with gratitude and appreciation.
As time passes and I get stronger and stronger, I am doing all I can to stay safe and regain my strength so that I would have a fighting chance of “making it.” I have a great appreciation for receiving “MY CHOICES: A Planner for Healing” as it helped me to remember who I am other than being defined by my cancer. It helped me to remember which things I had control over in light of so many things happening to me personally as well as the world around me. It may be a changing world, but I still want to be around to attend my daughter’s wedding and to see my other daughter graduate medical school. I feel blessed that my cancer was discovered early enough to remove it. Cancer and Coronavirus both have similar silver linings. Life is unpredictable, and I will do my best to live well each day I am given with gratitude and appreciation.
7
A few words from our Lung Cancer Program Director, Cindy Langhorne:
I enjoyed communicating with Robin in more detail about her experience with Lung Cancer and COVID, and her use of MY CHOICES: A Planner for Healing. What struck me was Robin’s understanding of her reality – the time is passing, and things are postponed due to the COVID virus. Robin hopes that she is around long enough to SEE and BE at the things that motivate her to get healthy. Robin’s bravery touched me, and I loved her willingness to think bigger than just the next year or two. I agree with Robin’s daughter, who said, “Robin will just have to live longer to SEE and BE at the things she planned for.”

Hildy Grossman, Founder of ULC
In the Fall of 2006, I bought a pair of green sandals with a cute kitten heel. I enjoyed the color and style and made sure they were comfortable, but it never occurred to me to examine the sole. Several days later, I put them on and headed down my basement stairs. One step onto the threshold and out went my feet as though I’d stepped onto ice: one foot went back and the other scraped the wall in front of me. Fortunately, the basement stairs are very narrow, and I was able to catch myself by grabbing both walls of the passageway.
1
Thus began an astonishing journey. After my narrow escape, I felt fine, except for some discomfort in my left wrist, elbow, and right ankle. I figured I should check myself out, primarily for the twinge in my left forearm. So, I began with a referral to see a hand surgeon who wanted to give me cortisone injections, but she wasn’t sure what site to use. Next, another hand specialist who wasn’t sure the problem had to do with my hand – maybe it was tennis elbow? My referral was to a neurologist to confirm a diagnosis, but he only tested for my wrist and not my elbow. He concluded there was no nerve damage in my wrist and ordered an MRI to see if I had a pinched nerve in my back. The MRI came back. It showed no pinched nerve – but it picked up two tiny spots in my right lung. My internist sent me for further tests and an eventual biopsy.
The diagnosis: lung cancer!
2
Fortunately, my Internist sent me to a top-notch surgeon, Dr. John Wain, at Massachusetts General Hospital, who scheduled my surgery three weeks later. Because of my early diagnosis, he was able to remove just the two small tumors in two lobes and a small section of tissue around the sites. They were small, early-stage, and contained – they hadn’t spread. My oncologist, Jennifer Temel, felt I didn’t need any further treatment as did her colleague, Dr. Tom Lynch, Chief of Thoracic Oncology.
My internist reflected on all the events that led to this fortunate outcome and said to me, “Somebody up there really likes you!”
I went home from the hospital to recuperate.
3
Most people would say there’s nothing fortunate about getting lung cancer. It was horrifying, shocking, and upsetting to wrestle with the diagnosis and try to figure out what it meant for my life and life expectancy. As I came to terms with it, I also found that the experience gave me a different level of awareness of how lucky I have been. My husband, Richard and daughter, Micaela went to all of my doctor’s visits with me. My son, David and his wife, Amy arranged for food to be delivered. My daughters Claire and Robin came from San Jose and Chicago to nurse me in the hospital, and when I came home. My dearest friends rallied to help me in every way possible, from researching the latest treatments and outcomes of lung cancer to bringing me dinner and keeping me company. Their extreme kindness made me vow to be a better friend to someone in need.
So many people expressed concern, good wishes, and a desire to be involved and updated about my recovery. I was so moved by how connected all of our lives are, even extending to good people we‘ve never met.
4
 Peter Jennings, ABC News Anchor, died of lung cancer at age 67.
Peter Jennings, ABC News Anchor, died of lung cancer at age 67.
All of us know someone who has had lung cancer. Most of us have stereotyped lung cancer: I know I have. It seemed like a disease reserved for older men who smoked for a lifetime. This isn’t true. It can happen to any one of us. This disease touches all of our lives. It might be a member of your family, a friend, or a neighbor. Perhaps you are a survivor. Or, maybe its someone you feel you know. Did you experience the same shock and unfairness I did when learning that Dana Reeves, a young non-smoker, died after years of heroically caring for her husband Christopher Reeves following his riding accident? Perhaps after inviting Peter Jennings into your home every evening to bring you the news, you, too were surprised by his illness and death. Remember how charming and funny Suzanne Pleshette was on The Bob Newhart Show? For me, no one had a voice like Beverly Sills. All of these well-known celebrities suffered and died from lung cancer.
5
That’s why early detection is so important.
In the days after I came home from the hospital, I worked to get my strength back. I did laps around my bedroom for exercise. I used my recovery time to reflect on my life, on what was important, and how to spend my time. I found inspiration through a book recommended to me by a tour guide, Tolga, whom I’d met while on vacation in Turkey. I emailed him about my lung cancer. He wrote back, quite unsentimentally, and said to read The Alchemist, a fable by Brazilian author Paulo Coelho. It’s a book about learning to read the omens strewn along life’s path and, above all, following our dreams.
This wise guide said it was for me to make something of my experience. After I finished reading the book, I realized that the key point was about transforming commonplace events into something of value, making something of each and every experience. This message spurred me to think about how I could find a way to make something worthwhile and life-affirming out of having had lung cancer, an experience that on the surface was of no value whatsoever.
6
The answer was Upstage Lung Cancer.
Creating Upstage Lung Cancer
My life has been about caring for people and bringing joy into their lives when I can. I have two professions. I am a clinical psychologist and I am a professional singer. As a psychologist, I have the honor of being invited into people’s lives and connecting at a deep level. As a singer, and a member of The Follen Angels (my jazz/cabaret group), the music is also about making meaningful connections. Our group has so much pleasure creating music together and then sharing our programs with enthusiastic audiences. Music ignites deep feelings and, often, important memories. For me, music is life-affirming. It’s therapeutic. Could I turn these skills and interests into something that could make a valuable contribution to raising awareness of lung cancer and its serious consequences, while supporting research on early detection and new treatments for this dreaded disease?
7
The birth of an idea
My reflections led to ideas about creating a musical theater event that could be used to raise money to benefit lung cancer research and raise awareness of our cause. I began to conceive of a show to feature the great showman, Florenz Ziegfeld. I shared this with my friend, Buck Spurr, producer, and entertainment consultant, who was immediately sold on the idea. Next, I turned to another dear friend, Crispin Weinberg, who, for many years, had served as producer for a show, Devotion Follies, we had worked on together in Brookline, Massachusetts. I asked him for his help with the new project, and he was eager to be there 100%. Finally, I called my writing partner, John Lamb, and asked him if he’d be willing to put our current project, a mystery novel, on hold to help me finish writing a musical theater show I’d begun called, Ziegfeld! He, too, was enthusiastically on board.
8
I met with nationally renowned Thoracic Oncologists Tom Lynch, MD, and Jennifer Temel, MD, at Massachusetts General Hospital Cancer Center in Boston, Massachusetts. We discussed the exciting and innovative research going on at the Massachusetts General Hospital Cancer Center, looking at early detection and new treatments for lung cancer. I told them I wanted to use the Ziegfeld! Project to raise funds to support these efforts. They couldn’t have been more enthusiastic.
Crispin and I contacted Susan Gessner, who, six months earlier, had been diagnosed with lung cancer in a very early stage, too. She happily agreed to serve as President of the Board of the non-profit organization we wanted to create. Our friend, Melissa Langa, an attorney, volunteered to help us with the papers, and we submitted the application in August 2008. From there, we contacted a group of dear friends with exceptional abilities and talents and asked them to serve on the Board of Directors of our new organization. We held our first Board meeting in September. Each member brings particular areas of expertise and energy to make us an effective, think-outside-of-the box organization. We also asked Tom Lynch, MD, Jennifer Temel, MD, and John Wain, MD, all outstanding specialists in the field of lung cancer to serve as a Medical Advisory Board. They each accepted with great enthusiasm.
9
Our Board of Directors agreed with my vision that we could do more if we created other shows as we work on producing Ziegfeld!. And so, our name Upstage Lung Cancer was born. In October 2008 we had our first fundraiser, a cabaret/jazz concert in a private home. The evening included a jazz performance by the Follen Angels and a very inspirational talk by Dr. Jennifer Temel. Dr. Temel discussed the status of lung cancer and her own work on the psychological aspects of living and dying with the disease. The event was a tremendous success, and we were planning a second, similar program on March 29, 2009.
I continue to be thrilled by the outpouring of help from professionals who volunteer their time and help. Robin Friedman at Visual Velocity continues to give us amazing graphic designs and creative website development support. Fatima Scipione at McK Healthcare helps us to think about fundraising and promoting our organization. Steve Biondolillo is helping us figure out how to raise lung cancer awareness so that it equals breast cancer awareness. Paula Davis, medical writer, and Annette Pringle, editor, make sure everything we write is of the highest quality. And there are many more wonderful volunteers helping us to make Upstage Lung Cancer to succeed.
10
The fact that I have had lung cancer is ever-present for me. My six month CT scans are wonderfully reassuring yet terrifying to anticipate. There is always that What if…? fear.
But, instead of focusing on “What if?” I want to put my considerable energy into working on our original Ziegfeld! Show and thinking about creating other exciting musical events. We are on our way.
We are using music and entertainment
the – elixir – of life to fight lung cancer.

Empowered
Written by a survivor determined to be a sur-THRIVE-er.
Jessica Steinberg, M.S.
in collaboration with Caring Ambassadors Program
In April 2011, when I was 39 years old, I received an injury that left me needing both an attorney and a chest x-ray.
One week later, I had signed divorce papers and found out I had lung cancer.
Click the arrows to view next slide

1


I don’t know how anybody can hear “you have cancer” without feeling like it deserves a string of expletives.
Let’s face it — no matter what stage of life you’re in, there is never a good time to hear those 3 words. So, let yourself have some time to deal with it. Cry, wail, scream, hop up and down, punch your pillow, blame yourself, sob, blame everybody else, rail against the universe, attempt to write your obituary, and/or whatever else you need to do.


2
At some point, though, you are going to have to face it.
It’s time to make some choices.
You have to do SOMETHING — even if it’s choosing to do nothing.


4
It really helped ME to define my priorities and my options first. This was easy for me — my 2 boys were my first priority. That made my choice clear to me. I was going to fight like crazy so I could raise them. (It was mildly tempting to choose ‘drink myself to death’, but that wasn’t really the legacy I wanted to leave behind.) It really helps me to keep my sons in the forefront of my mind when I think about my cancer.
What drives YOUR decision?
Assuming you made the choice to fight, WHO or WHAT are you fighting for?
I’ve had other patients tell me all kinds of reasons they are motivated to fight — and everyone is different. Often it is about family — whether it’s a partner, children, grandchildren, and sometimes pets. I’ve heard from some that it’s the work they do that inspires them.


5
Another person said they just ‘aren’t ready’ to be done living. They still want to go sky-diving, Rocky Mountain climbing, and 2.7 seconds on a bull named Fu Man Chu. (Okay, it was actually Tim McGraw that said that, but you never know… that might be some peoples’ reasons.)
So, if you’re with me… it’s time to put your ‘brave boots’ on. In the next few pages, I am going to share with you what got ME this far and how I became an “empowered” patient.


6
Just know, though, that it is up to you.
This is YOUR cancer journey
and YOU are in charge of what happens next.
7


8


9


- I chose an oncologist who specializes in my type of cancer & got second opinions. If available, a doctor that has your cancer as a specialty ensures that your treatment is consistent with the newest research and treatment protocols.
- I established a working relationship of mutual trust, respect, and clear communication.Empowered patients recognize that their doctor is just a person, too — kindness counts on both sides. Empowered patients use their appointment time wisely. They arrive prepared with any questions or feedback and follow physician and prescription directions. They ask questions when they don’t understand something or need explanations.


9b
- I became an active partner in my own care. Empowered patients insist on a biopsy or testing on their tumor for biomarkers that can determine treatment. They are invested in knowing their treatment options and are a partner in the decision-making process. They make sure they clearly understand the expected benefits and potential side effects of all options.

10
- I became my own best advocate. A positive working relationship with your oncologist does not change the fact they likely have patient loads in the hundreds, if not thousands. An empowered patient has just ONE — themselves. They don’t hesitate to ask for copies of their reports, get second opinions, or seek out further information.
- I realized that caregivers are heroes, too. Having supportive people along with you through cancer makes a difference that is indescribable. Let them in. Soak up their support and offers to help. Learn and practice saying “yes” and experience the power of love and community. Caregivers truly teach us that no one fights alone.
11
- I explored the world of palliative care. Palliative care focuses on providing patients with relief from the symptoms and stress of cancer. The goal is to improve quality of life for both the patient and the family. Empowered patients use these services to focus on feeling as well as possible.
![]()
![]()
- I realized the importance of good mental/emotional health. An empowered patient understands that the cancer journey includes challenging and emotional times. They recognize there are many strategies for maintaining good mental and emotional health and seek the best option for them.
12
- I sought balance. An empowered patient learns to fuel their body healthfully, while recognizing that participating fully in social activities and family celebration may have more health benefits than avoiding nightshade vegetables. An empowered patient stays as active as they are able, understands that treatment takes a toll on their body, and allows time for rest and relaxation. Sleep is healing!
- I realized that Kenny Rogers may have been on to something. Empowered patients know that you DO need to know when to hold ‘em, know when to fold ‘em, know when to walk away and know when to run. A cancer diagnosis has a funny way of changing one’s perspective on what really matters. I realized I couldn’t just learn and practice saying “yes” — sometimes I needed to say “no” too. I focused on saying “YES” to experiences or relationships that brought joy and happiness to my life, and “NO” to situations or relationships that had a negative impact or brought toxicity to my life.
13
- I maintained my sense of humor. Jest for the health of it! Seriously — there are studies that associate laughter with increased health benefits. Humor helps overcome and cope with the daily trials. When you find a way to laugh during stressful times, you automatically shift toward a frame of mind that invites an outlook of hope and a conviction that you can beat this @!*#. I committed to my boys early on that we would find some joy and humor in each day. There may have been several pajama drive-through trips for milkshakes and lots of movie nights, but I’d like to think we did it.
- I sought out and found a cancer community. Connecting with other survivors is like a power boost! Whether it be through a formal “mentor” program, an actual or virtual support group, attending/hosting awareness and advocacy events, blogging — there’s just something special about being with other survivors that “get you” like no one else can . Plus, it’s a great way to stay current with emerging research and treatment. Thanks to the internet and social media, you can be active in community-building while sitting on the couch. Be sure to let your caregiver know that there are groups for them, too!
14




15
Empowered patients know that having hope is a choice they can make. Hope is the belief that a positive outcome is ahead.
And let it be clear –
HOPE IS NOT DENIAL


16
It is educated optimism, and empowered patients know there has never been a time in the world of cancer treatment where having hope is so warranted.
Hope can inspire you to action, including being a stronger advocate for yourself and others.
Hope is contagious — when you have the spirit of hope guiding you through this journey, you may find that it affects the whole world you live in, your relationships with others, your dreams, and your goals and wishes for the future.
17

18


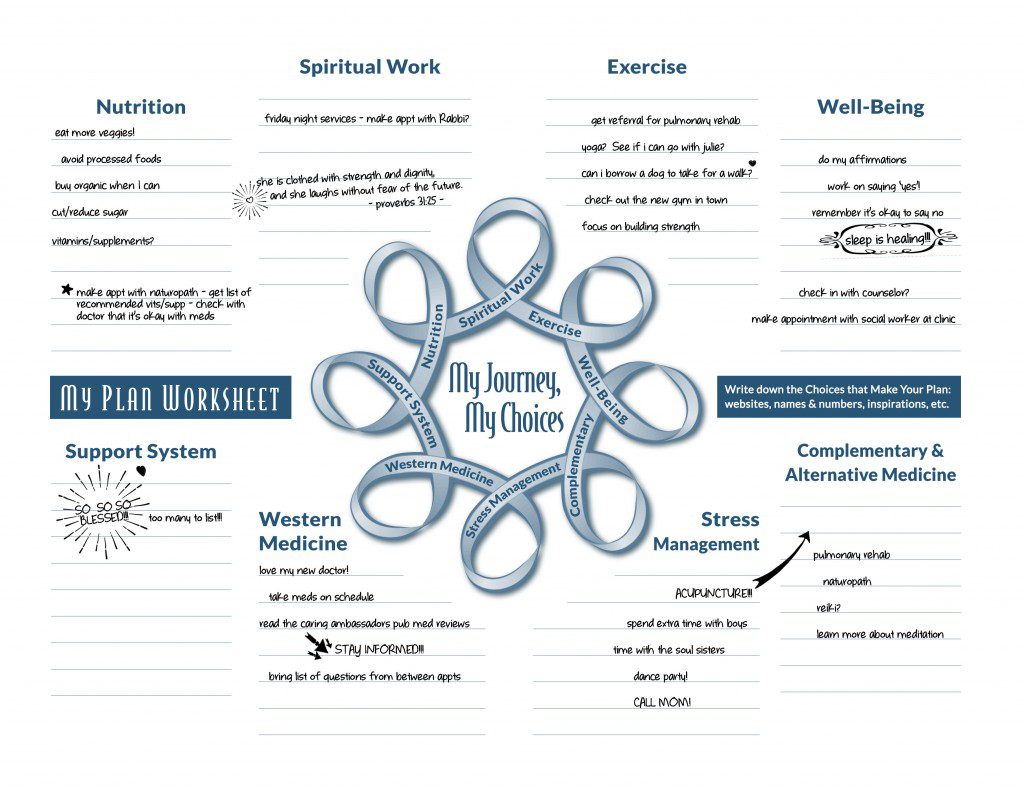
Research has shown that using positive self-talk reduces stress and depression, improves coping skills, and may even effect health outcomes. What *is* positive self-talk? It’s the voice in our head that narrates throughout our day. It’s like an inner sports announcer!
All the emotions of a cancer diagnosis can make it difficult to keep our self-talk positive. Consider the possibilities of writing yourself a note of affirmation and posting it somewhere where you’ll see it often, or your favorite inspiring quote on your mirror, or explore your creative side to create art for your home. The more you see or experience these words, the easier it is to keep your self-talk positive.
You are welcome to download and print any images to get you started. Ultimately, though, you should have something that is meaningful to YOU.



A Note from the Author:
Thank you for your consideration of this material and I hope that sharing what I have learned will be of some use to you. I would love to hear *your* stories of empowerment! Feel free to contact me through Caring Ambassadors at mystory@CaringAmbassadors.org
Remember: This is YOUR cancer journey and YOU are in charge of what happens next. YOU can do it!!!
Jessica Steinberg, M.S.
Download Jessica’s Story here: Empowered! My Journey My Choices PDF
Download your own My Integrative Health Care Plan Worksheet PDF
Caring Ambassadors 2020 © ALL RIGHTS RESERVED


Ain’t No Mountain High Enough – Marvin Gaye & Tami Terrell
Best Day of My Life – American Authors
Dog Days are Over – Florence and the Machine
Down – Jay Sean
Eye of the Tiger – Survivor
Fight Song – Rachel Platten
F**k You (or clean version Forget You) – Cee Lo Green
Happy – Pharrell Williams
I Will Survive – Gloria Gaynor
Joy to the World – Three Dog Night
On Top of the World – Imagine Dragons
Roar – Katy Perry
Say Hey (I Love You) – Michael Franti & the Spearheads
Shake it Off – Taylor Swift
Stronger – Kelly Clarkson
The Fighter – Gym Class Heroes
The Gambler – Kenny Rogers
Tubthumpin’ – Chumbawamba
Whip it – Devo
You Ain’t Seen Nothing Yet – Bachmann Turner Overdrive
Ready to share your story?
The Lung Cancer Program team has started collecting stories, and we want to include YOU! Would you be so kind as to share a snippet about your lung cancer experience with us? There is no right way to share – talk, write, draw, speak poetry – just please SHARE
